A few years ago, I volunteered at a community health clinic that served low-income families, and that experience truly opened my eyes to what health equity means in real life. I saw how access to healthcare, transportation, and even language barriers could determine someone’s quality of care. Witnessing patients finally receive fair treatment regardless of their background showed me how essential equitable health systems are. It reminded me that health equity isn’t just a policy, it’s about dignity, opportunity, and justice for every person.
Health equity means ensuring everyone has a fair and just opportunity to achieve optimal health, regardless of socioeconomic status, race, gender, or location, by removing barriers that prevent equal access to healthcare resources.
In this article we will discuss “Health equity.”
Understanding the Concept of Health Equity
Health equity refers to the fair distribution of healthcare resources, opportunities, and outcomes across all segments of society. It means ensuring that everyone regardless of race, gender, income, geography, or education has the opportunity to achieve their highest level of health.
For example, a rural population may need more mobile clinics or telemedicine services than an urban population to achieve similar health outcomes. In this sense, health equity isn’t about sameness it’s about fairness.
At its core, achieving health equity requires eliminating barriers such as poverty, systemic discrimination, lack of education, and inadequate access to medical care. These barriers create unfair differences in how long and how well people live. A truly equitable health system recognizes these differences and takes deliberate action to close the gaps.
Health Equity vs. Health Equality: Understanding the Difference

source:ationalrn
Although health equity and health equality are often used interchangeably, they are fundamentally different in philosophy and approach.
Health equivalency means furnishing the same coffers and openings to everyone. Health equity, on the other hand, focuses on distributing coffers according to individual and community needs so that issues are fair, not just invariant.
| Aspect | Health Equality | Health Equity |
| Definition: | Everyone receives the same healthcare resources | Resources are distributed based on individual or community need |
| Goal: | Uniform treatment | Fair outcomes |
| Approach: | Assumes equal starting points | Recognizes pre-existing disadvantages |
| Example: | Each city gets the same number of doctors | Underserved areas get additional healthcare support |
In simple terms, equality promotes sameness, while equity promotes fairness. For healthcare systems to progress, policies must be designed with equity at their core rather than uniformity.
The Social Determinants of Health (SDOH)
Health is not determined solely by medical care or genetics. In fact, most health outcomes are influenced by what are called the Social Determinants of Health (SDOH) the conditions in which people are born, grow, live, work, and age.
Research shows that up to 80% of health outcomes are influenced by these non-medical factors. That means improving health equity requires focusing on improving living conditions, not just hospitals and clinics.
Key Social Determinants Include:
- Economic Stability: Income determines access to healthy food, quality housing, and medical care. Financial insecurity often leads to chronic stress and poor health.
- Education Access and Quality: Education shapes health literacy, job opportunities, and the ability to make informed health decisions.
- Healthcare Access and Quality: Access to affordable and high-quality healthcare services determines how early illnesses are detected and treated.
- Neighborhood and Built Environment: Safe, clean, and well-designed neighborhoods encourage physical activity and reduce exposure to pollutants.
- Social and Community Context: Supportive relationships and social inclusion improve both mental and physical well-being.
To achieve health equity, policies must address these determinants directly through better housing, education, income opportunities, and community infrastructure.
The Role of Policy in Promoting Health Equity

source: wdtrust.org.uk
Governments and health organizations play a central role in building systems that promote equity over inequality. Effective policy must go beyond funding hospitals and clinics—it must target the root causes of health disparities.
Key Policy Strategies Include:
- Expanding Healthcare Coverage: Programs like Medicaid expansion or universal health coverage ensure that no one remains uninsured.
- Implementing Value-Based Care: Instead of rewarding quantity, healthcare systems should reward quality and positive patient outcomes.
- Cultural Competence Training: Healthcare professionals must understand diverse backgrounds and reduce unconscious bias.
- Investment in Preventive Care: Preventing illness is far more effective and equitable than treating it after it occurs.
- Cross-Sector Integration: Policies that promote fair housing, education, and minimum wages indirectly strengthen public health.
When public policy focuses on social justice and inclusion, healthcare becomes not a privilege, but a human right available to all.
Health Equity in the Global Context
Health equity is not just a national issue it’s a global challenge. Around the world, healthcare systems face massive inequalities in access, quality, and affordability.
The World Health Organization (WHO) emphasizes “Health for All” through its Universal Health Coverage (UHC) initiative. However, achieving this vision remains a struggle for many countries.
Examples of Global Inequities:
- Sub-Saharan Africa: Only 3% of the world’s healthcare professionals serve over 11% of the global population.
- Indigenous Populations: Across continents, Indigenous communities suffer higher rates of chronic diseases and shorter life expectancy.
- Pandemic Response: During COVID-19, vaccine distribution revealed a stark global divide wealthier nations vaccinated faster, leaving poorer regions behind.
Addressing global health inequities requires coordinated action, ethical responsibility, and investment from wealthier nations to build sustainable healthcare infrastructures.
Barriers to Achieving Health Equity
Even with widespread awareness, significant barriers persist in the path toward achieving equitable health outcomes.
1. Socioeconomic Inequality
Poverty remains one of the most influential predictors of poor health. Low-income communities often face unhealthy environments, inadequate nutrition, and limited healthcare access.
2. Racial and Ethnic Disparities
Systemic racism and cultural bias can affect diagnosis, treatment quality, and patient trust in healthcare systems. This leads to unequal treatment and worse outcomes for marginalized groups.
3. Geographic Disparities
Rural and remote areas frequently lack medical infrastructure, specialists, and emergency services, resulting in delayed treatment.
4. Education and Health Literacy
A lack of education prevents individuals from understanding health information, leading to poor prevention and treatment decisions.
5. Policy Gaps
Underfunded public systems and inconsistent data collection perpetuate inequality, making it difficult to design effective, data-driven interventions.
Technology and Health Equity

source:americanmedicalcompliance
Technology has the potential to revolutionize access to care but it must be implemented thoughtfully to avoid increasing the digital divide.
Telemedicine
Telehealth connects patients to doctors remotely, particularly benefiting rural populations. However, disparities in internet access and digital literacy still limit its reach.
Data Analytics and Artificial Intelligence
AI helps healthcare systems detect trends, allocate resources efficiently, and identify at-risk populations. Yet, biased data can lead to unequal results if diversity isn’t built into algorithms.
Wearable Health Devices
Smart devices allow individuals to track their health metrics in real-time, promoting preventive care. However, cost barriers prevent many from benefiting from such technologies.
To truly enhance health equity, technological innovation must focus on accessibility, affordability, and inclusion.
Health Equity in the Private Sector
Private companies and healthcare organizations are increasingly integrating equity-driven initiatives into their operations. They recognize that healthy employees and communities contribute to sustainable business success.
Examples of Private Sector Initiatives:
- Diversity, equity, and inclusion (DEI) programs that combat workplace bias.
- Employee wellness initiatives emphasizing mental health and chronic disease prevention.
- Equitable healthcare benefits covering maternity, disability, and mental health care.
- Partnerships with local communities to enhance outreach and education.
When companies promote health equity, they not only improve public health but also build stronger, more loyal workforces and communities.
The Economic Impact of Health Equity
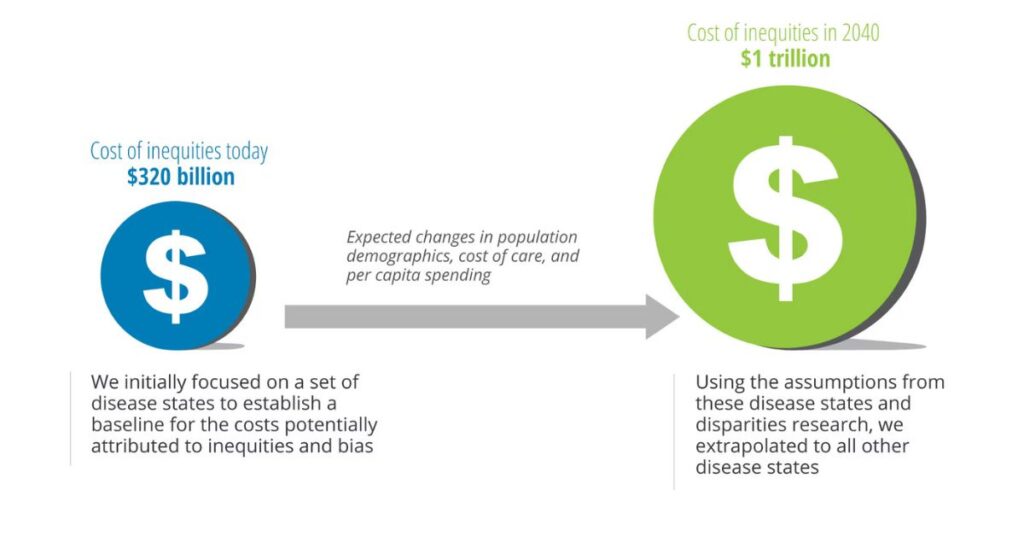
source: deloitte
Health equity is not just an ethical imperative it’s an economic necessity. Health disparities result in billions of dollars lost every year through reduced productivity, higher healthcare costs, and premature deaths.
According to the National Academies of Sciences, eliminating health inequities could save the U.S. economy over $230 billion annually. Investing in equity-driven policies provides measurable benefits:
- Fewer emergency hospitalizations
- Greater workforce participation
- Higher educational and employment performance
- Stronger community resilience during crises
Promoting equity is therefore not only morally right but also fiscally smart it’s an investment in both human and economic potential.
Measuring Progress: Metrics and Indicators
Assessing progress toward health equity requires reliable, disaggregated data. Metrics help policymakers identify disparities and track improvements.
Common Health Equity Indicators:
- Life expectancy and mortality rates by demographic group
- Chronic disease prevalence across income levels
- Access to preventive and primary healthcare
- Infant and maternal mortality rates by region
- Patient satisfaction and perceived care quality
Transparent reporting and community engagement ensure accountability, while data-driven decision-making helps target interventions where they’re most needed.
The Role of Education in Health Equity

source: easyuni
Education serves as a foundation for long-term health equity. Individuals with higher education levels generally have better access to jobs, income stability, and health awareness.
Schools and universities can foster equity through:
- Health literacy and nutrition programs
- Access to mental health support services
- Early education opportunities in underserved communities
When education systems focus on inclusion, they empower individuals to make informed health decisions and advocate for themselves creating generational progress toward health equity.
Strategies to Promote Health Equity
To make equitable healthcare a reality, both governments and communities must collaborate across multiple levels.
1. Community Engagement
Local communities understand their needs best. Including them in decision-making ensures culturally relevant, sustainable solutions.
2. Cross-Sector Collaboration
Public health, education, transportation, and housing must work together to address interconnected social determinants.
3. Culturally Competent Care
Healthcare professionals must learn to recognize and respect diverse cultural beliefs and communication styles.
4. Data-Driven Decision Making
Using accurate, disaggregated data reveals disparities and guides better policy design.
5. Empowerment and Advocacy
Grassroots movements that empower marginalized groups help drive lasting systemic reform.
The Future of Health Equity: A Vision for 2030 and Beyond
The coming decade offers a pivotal opportunity to reshape healthcare systems around equity, transparency, and inclusion. Global initiatives like the UN Sustainable Development Goal 3 (Good Health and Well-being) and the WHO Health Equity Assessment Toolkit serve as guiding frameworks.
By 2030, the vision is clear: universal access to care, ethical use of technology, and the elimination of discrimination within health systems. Achieving this future requires shared responsibility between governments, private sectors, and communities.
Frequently Asked Questions:
1. What is the meaning of HealthEquity?
HealthEquity means ensuring that everyone has fair access to healthcare opportunities and resources, regardless of their income, race, or background, by removing social and economic barriers to health.
2. What is an example of HealthEquity?
An example of health equity is providing additional healthcare funding and mobile clinics in rural areas so that underserved populations receive the same level of care as urban communities.
3. What do the HealthEquity do?
HealthEquity is a company that helps individuals manage their health savings accounts (HSAs), flexible spending accounts (FSAs), and other health benefit plans to make healthcare spending and saving easier and more efficient.
4. Can I cash out my HealthEquity account?
You can withdraw funds from your HealthEquity HSA at any time, but if used for non-qualified expenses before age 65, the withdrawal is subject to income tax and a penalty.
5. What is the HealthEquity controversy?
Some controversies around HealthEquity relate to customer service concerns and confusion over eligible expenses, though the company generally maintains strong compliance with IRS and healthcare regulations.
6. Is HealthEquity a health insurance?
No, HealthEquity is not a health insurance provider. It’s a financial services company that manages tax-advantaged accounts like HSAs, HRAs, and FSAs to help individuals pay for medical expenses.
7. What can I spend my HealthEquity on?
You can use your HealthEquity HSA funds for IRS-approved qualified medical expenses such as doctor visits, prescriptions, dental care, vision care, and certain over-the-counter health items.
8. What are the benefits of HealthEquity?
HealthEquity offers tax advantages, convenient healthcare spending, investment opportunities for unused funds, and easy digital account management to help individuals maximize their healthcare savings and spending efficiency.
9. What is another name for HealthEquity?
HealthEquity is often referred to as an HSA provider or health savings account administrator, as it primarily helps people manage and grow their healthcare-related financial accounts.
10. Can I use my HealthEquity card at the doctor’s office?
Yes, you can use your HealthEquity debit card at most doctor’s offices, pharmacies, and clinics to pay directly for eligible medical expenses covered under your health savings account.
Conclusion:
Health equity represents the foundation of a just and sustainable healthcare system where everyone, regardless of their background, has the opportunity to live a healthy life. It calls for removing systemic barriers such as poverty, discrimination, and unequal access to care. Achieving health equity requires collaboration across governments, communities, and the private sector, focusing on policies that promote fairness, inclusion, and accessibility. As technology, education, and policy evolve, societies must ensure progress benefits everyone equally. Ultimately, health equity is not just a healthcare goal it’s a moral and social commitment to dignity, justice, and shared well-being for all.

Leave a Reply